
Hypnotherapy, imagine reducing chronic pain without medication, managing IBS symptoms more effectively than dietary restrictions alone, or helping children overcome needle phobia in just a few sessions. Hypnotherapy delivers these outcomes through a scientifically validated approach that harnesses the brain's capacity for focused attention and suggestion. As mainstream medical guidelines increasingly recommend hypnotherapy for conditions ranging from irritable bowel syndrome to surgical anxiety, working professionals are discovering both clinical applications and career opportunities in this evidence-based therapeutic modality.
Key Takeaways
- Hypnotherapy uses guided relaxation and focused attention to access the subconscious mind, enabling behavioural and physiological changes backed by neurological evidence
- Anxiety and stress management accounts for 52% of global hypnotherapy demand, making it the most established clinical application [1]
- Gut-directed hypnotherapy is now recommended in American and European gastroenterology guidelines as a second-line treatment for IBS alongside cognitive behavioural therapy [1]
- Meta-analysis shows hypnotherapy participants reduced anxiety more than 79% of control participants, with effects sustained at follow-up [1]
- Professional certification requires foundation training (typically 120-450 hours), supervised practice, and registration with recognized bodies
- Chronic pain management shows medium to large effect sizes (d = 0.5 to 2.72), with minimum eight-session protocols producing optimal outcomes [1]
- Pediatric applications demonstrate some of the largest effect sizes, particularly for needle-related procedures and pre-surgical anxiety [1]
- No significant adverse events have been reported across studies from 2018-2026, establishing hypnotherapy's excellent safety profile [3]
- Specialized niches including performance enhancement, medical procedure anxiety, and sleep disorders show growing clinical demand
- Career pathways include private practice, healthcare integration, corporate wellness programs, and specialized medical referral networks
Quick Answer
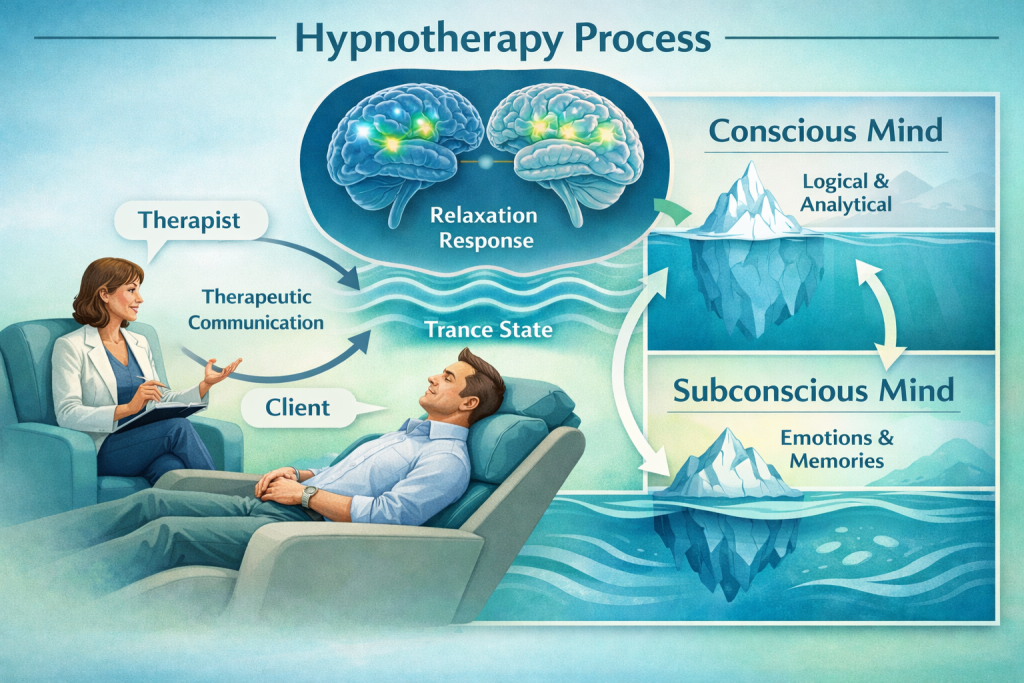
Hypnotherapy is a therapeutic technique that uses guided relaxation, focused attention, and verbal suggestion to access heightened states of awareness where behavioural and physiological changes become more achievable. Unlike stage hypnosis entertainment, clinical hypnotherapy is an evidence-based intervention now recommended in medical guidelines for conditions including irritable bowel syndrome, chronic pain, anxiety disorders, and perioperative care. Professional practice requires accredited training (typically 120-450 hours), supervised clinical experience, and registration with bodies such as the General Hypnotherapy Register or National Council for Hypnotherapy in the UK.
What Is Hypnotherapy and How Does It Work?
Hypnotherapy is a therapeutic intervention that induces a trance-like state of focused attention, heightened suggestibility, and deep relaxation to facilitate psychological and physiological changes. During this state, the conscious critical faculty becomes less active while the subconscious mind becomes more receptive to therapeutic suggestions aligned with the client's goals.
The process works through several neurological mechanisms. Brain imaging studies reveal that hypnotic states produce measurable changes in neural activity, particularly in areas governing attention, sensory processing, and emotional regulation. When a qualified hypnotherapist guides a client into trance, the brain's default mode network shows altered connectivity patterns that enhance the effectiveness of therapeutic interventions.
Key components of clinical hypnotherapy include:
- Induction: Techniques that guide clients from normal waking consciousness into a focused, relaxed state
- Deepening: Methods that enhance the trance state to increase receptivity to therapeutic work
- Suggestion: Carefully crafted verbal communications targeting specific therapeutic goals
- Imagery: Visualization techniques that engage the subconscious mind in problem-solving
- Reframing: Cognitive restructuring that occurs more readily in the hypnotic state
- Post-hypnotic suggestions: Instructions that continue influencing behaviour after the session ends
Common misconception: Clients remain fully aware and in control during hypnotherapy. You cannot be made to do anything against your values or will. The hypnotic state resembles the focused absorption experienced when deeply engaged in a book or film, not unconsciousness or sleep.
Choose hypnotherapy if you're seeking evidence-based support for anxiety, chronic pain, IBS, sleep disorders, or habit change, and prefer non-pharmacological interventions. It works best when combined with genuine motivation for change and willingness to engage with the therapeutic process.
What Conditions Does Hypnotherapy Treat Most Effectively?
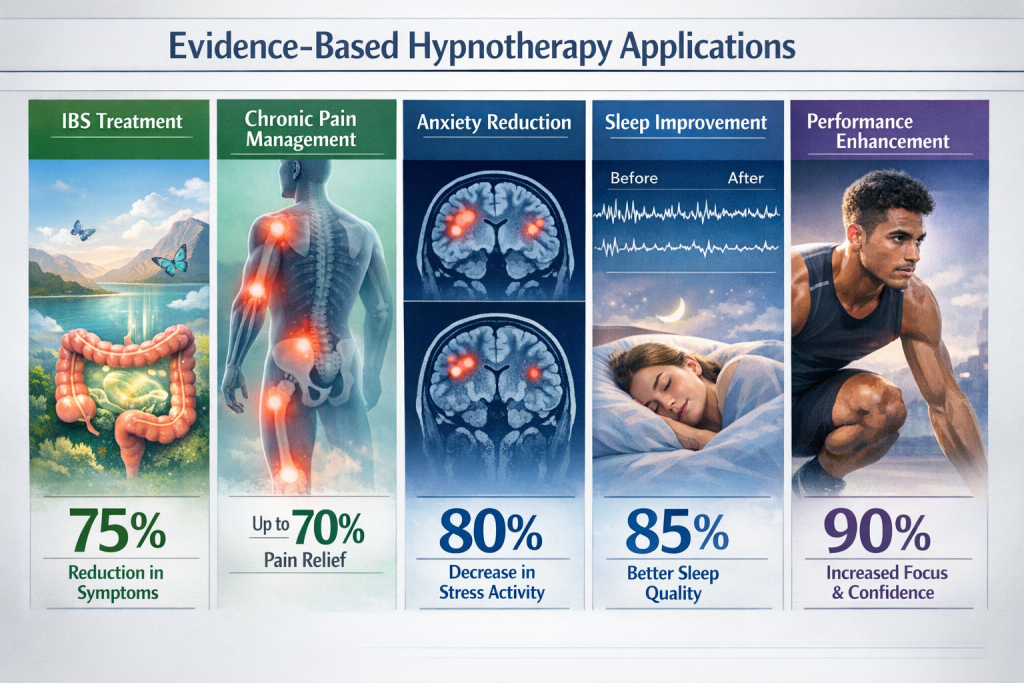
Hypnotherapy demonstrates the strongest clinical evidence for anxiety disorders, irritable bowel syndrome, chronic pain, sleep disturbances, and perioperative care. Recent systematic reviews confirm these applications meet rigorous scientific standards, with effect sizes ranging from medium to large across multiple conditions.
Anxiety and Stress Management
Anxiety represents the largest clinical application, accounting for approximately 52% of all hypnotherapy demand globally [1]. Meta-analysis published in the International Journal of Clinical and Experimental Hypnosis demonstrates that participants receiving hypnosis reduced anxiety more than approximately 79% of control participants, with follow-up assessments showing 84% greater improvement than control groups [1].
Hypnotherapy addresses anxiety through multiple pathways: direct symptom reduction via relaxation responses, cognitive reframing of anxiety-triggering thoughts, and desensitization to specific anxiety triggers. The approach proves particularly effective for generalized anxiety disorder, social anxiety, and performance anxiety.
Irritable Bowel Syndrome (IBS)
Gut-directed hypnotherapy represents what specialists call "the breakout specialty of the decade" [1]. The American College of Gastroenterology's clinical guidelines now recommend gut-directed psychotherapy for treating global IBS symptoms, with European and North American gastroenterology guidelines specifically recommending gut-directed hypnosis as a second-line treatment option alongside cognitive behavioural therapy [1].
A 2025 systematic review and meta-analysis in Neurogastroenterology & Motility confirmed that gut-directed hypnotherapy may improve global symptoms of IBS, with particular effectiveness for pain symptoms compared to other standard interventions [1]. A 2016 Monash University study found that gut-directed hypnotherapy was equally effective as the low FODMAP diet for managing IBS symptoms while being more effective at improving psychological measures [1].
Gastroenterologist referrals are increasing as more GI doctors become aware of these clinical guidelines. Research published in the American Journal of Gastroenterology shows that patients referred by healthcare providers demonstrate better program adherence and outcomes [1].
Chronic Pain Management
Chronic pain management shows robust clinical evidence, with a 2024 study published in Frontiers in Psychology confirming that clinical hypnosis represents an efficient non-pharmacological intervention for pain management across various clinical populations [1]. Meta-analysis research found that a minimum of eight sessions produced significantly better outcomes than shorter treatment courses for musculoskeletal and neuropathic chronic pain [1].
A 2024 systematic review confirms adjunctive hypnosis produces clinically relevant analgesic effects, with neurophysiological studies revealing that hypnotic analgesia has clear effects on brain and spinal-cord functioning, providing objective evidence beyond placebo [1].
Edge case: Hypnotherapy works best for chronic pain when integrated with conventional medical care rather than used as a standalone replacement. Always maintain medical supervision for serious pain conditions.
Sleep Disorders
Sleep disorders show significant improvement with hypnotherapy intervention. A meta-analysis in Complementary Therapies in Medicine found that hypnotherapy significantly shortened sleep latency compared to waitlist controls [1]. For children, a retrospective chart review of 84 children and adolescents with insomnia found that 90% reported reduction in sleep onset time following hypnosis, and 52% reported no longer waking at night [1].
Emerging High-Value Applications
Recent research identifies several specialized applications showing strong outcomes:
- Pediatric procedures: Children undergoing needle-related procedures demonstrate some of the largest effect sizes for hypnosis intervention, alongside pre-surgical anxiety management and oncology support applications [1]
- Performance anxiety: Research published in Frontiers in Psychology shows hypnosis received before competition effectively reduced competitive anxiety and stress in athletes [1]
- Medical procedure anxiety: A 2025 systematic review confirmed hypnosis significantly reduced anxiety during invasive medical procedures, with virtual reality-enhanced hypnosis showing the most benefit [1]
How Does Hypnotherapy Compare to Other Therapeutic Approaches?
Hypnotherapy demonstrates outcomes for depression comparable to or exceeding cognitive behavioural therapy (CBT), with sustained benefits extending up to 3.5 years post-treatment [3]. Effect sizes range from medium to large (d = 0.5 to 2.72) across various conditions including chronic pain, anxiety disorders, and perioperative care [3].
| Comparison Factor | Hypnotherapy | Cognitive Behavioural Therapy | Medication |
| Typical Duration | 4-12 sessions for most conditions | 12-20 sessions typically | Ongoing as prescribed |
| Mechanism | Subconscious restructuring via suggestion | Conscious thought pattern modification | Biochemical intervention |
| Anxiety Effect Size | 79% improvement vs control [1] | Well-established, similar outcomes | Varies by medication class |
| IBS Effectiveness | Equal to low FODMAP diet, better psychological outcomes [1] | Recommended second-line treatment | Symptom-specific relief |
| Chronic Pain | Minimum 8 sessions optimal [1] | Standard approach, requires ongoing practice | Risk of dependency with opioids |
| Adverse Events | None reported (2018-2026) [3] | Minimal, occasional temporary distress | Varies, can be significant |
| Long-term Sustainability | Benefits sustained 3.5+ years [3] | Requires continued skill application | Typically requires ongoing use |
Choose hypnotherapy if: You prefer non-pharmacological approaches, have conditions with strong evidence bases (IBS, anxiety, chronic pain), or haven't responded adequately to conventional treatments alone.
Choose CBT if: You prefer structured, conscious cognitive work, need treatment for conditions with less hypnotherapy research, or prefer the extensive insurance coverage CBT typically receives.
Combine approaches when: Maximum benefit is the priority. Many practitioners integrate hypnotherapy with CBT techniques, creating cognitive hypnotherapy that leverages both modalities' strengths.
Common mistake: Viewing hypnotherapy as "alternative medicine" rather than an evidence-based complementary approach. Recent systematic reviews establish hypnosis as a credible, evidence-based healing modality warranting broader integration into mainstream clinical practice as a non-pharmacological treatment option [3].
What Qualifications and Training Do Professional Hypnotherapists Need?
Professional hypnotherapy practice in the UK requires completion of accredited training programs, supervised clinical practice hours, and registration with recognized professional bodies. Unlike some countries, the UK does not legally regulate hypnotherapy, making voluntary professional registration essential for credibility and insurance coverage.
Foundation Training Requirements
Accredited hypnotherapy training typically ranges from 120 to 450 hours depending on the certification level and specialization. Programs must cover:
- Theoretical foundations: Hypnotic phenomena, trance states, suggestibility, neurological mechanisms
- Induction techniques: Multiple approaches for guiding clients into therapeutic trance states
- Therapeutic interventions: Condition-specific protocols for anxiety, pain, habits, phobias, and other applications
- Clinical skills: Assessment, treatment planning, session structure, record-keeping
- Ethics and professional practice: Confidentiality, scope of practice, referral protocols, professional boundaries
- Supervised practice: Direct client work under qualified supervision (typically 50-100 hours minimum)
Professional Registration Bodies
In the UK, the main professional bodies include:
- General Hypnotherapy Register (GHR): Requires minimum 120 hours training from accredited schools
- National Council for Hypnotherapy (NCH): Requires completion of NCH-accredited diploma programs
- British Society of Clinical Hypnosis (BSCH): Requires healthcare professional background plus specialized hypnosis training
- Complementary and Natural Healthcare Council (CNHC): Government-supported voluntary register requiring accredited training
Choose BSCH if: You're already a healthcare professional (doctor, psychologist, nurse) seeking to add hypnotherapy to your clinical toolkit.
Choose GHR or NCH if: You're entering hypnotherapy as a primary career without prior healthcare credentials.
Specialized Advanced Training
After foundation certification, many practitioners pursue specialized training in high-demand niches:
- Gut-directed hypnotherapy: Specialized protocols for IBS and digestive disorders (typically 20-40 additional hours)
- Chronic pain management: Advanced pain control techniques and medical collaboration (30-50 hours)
- Pediatric hypnotherapy: Child-specific approaches and developmental considerations (20-40 hours)
- Performance enhancement: Sports psychology and performance anxiety applications (20-30 hours)
- Clinical hypnotherapy: Advanced integration with psychotherapy for complex presentations (100+ hours)
Edge case: Healthcare professionals (doctors, nurses, psychologists) can often complete shorter specialized hypnotherapy training (50-100 hours) since they already possess clinical assessment and treatment planning skills. Non-healthcare practitioners need more comprehensive foundational training.
Continuing Professional Development (CPD)
Professional bodies require ongoing CPD to maintain registration, typically 12-25 hours annually. CPD activities include advanced training workshops, supervision, peer consultation groups, conference attendance, and relevant reading.
For those seeking to build essential professional skills, hypnotherapy training develops competencies highly valued across healthcare and wellness sectors.
What Does a Typical Hypnotherapy Session Involve?
A standard hypnotherapy session lasts 50-90 minutes and follows a structured format designed to maximize therapeutic benefit while maintaining client safety and comfort. Understanding this structure helps prospective clients know what to expect and helps professionals deliver consistent, effective interventions.
Initial Consultation and Assessment
The first session typically dedicates 30-40 minutes to comprehensive assessment:
- Presenting problem: Detailed exploration of the issue bringing the client to therapy
- History: Relevant medical, psychological, and social background
- Goals: Specific, measurable outcomes the client wants to achieve
- Expectations: Discussion of what hypnotherapy can and cannot accomplish
- Contraindications screening: Identifying any conditions requiring medical clearance
- Informed consent: Explaining the process, addressing concerns, obtaining agreement
Common mistake: Rushing into hypnotic work without adequate assessment. Effective hypnotherapy requires understanding the client's unique situation, learning style, and therapeutic needs.
The Hypnotic Process
Following assessment, the therapist guides the client through several distinct phases:
1. Pre-talk and preparation (5-10 minutes)
- Explaining what will happen during the session
- Addressing any remaining concerns or questions
- Establishing comfort and rapport
- Setting the therapeutic frame
2. Induction (5-15 minutes)
- Guiding the client from normal waking consciousness into focused relaxation
- Using techniques matched to the client's responsiveness (progressive relaxation, eye fixation, rapid inductions, conversational approaches)
- Monitoring client responses through observable indicators
3. Deepening (3-8 minutes)
- Enhancing the trance state to increase therapeutic receptivity
- Using techniques like counting, imagery, or fractionation
- Establishing depth appropriate to the therapeutic work planned
4. Therapeutic intervention (15-30 minutes)
- Delivering condition-specific therapeutic work
- Using suggestion, imagery, reframing, or regression as appropriate
- Addressing the core issues identified in assessment
- Installing post-hypnotic suggestions for ongoing benefit
5. Emergence (2-5 minutes)
- Gradually returning the client to normal waking consciousness
- Ensuring full alertness and orientation
- Checking the client's experience and wellbeing
6. Debriefing (5-10 minutes)
- Discussing the session experience
- Providing any relevant homework or practice suggestions
- Scheduling follow-up sessions
- Answering questions
Number of Sessions Required
Treatment duration varies by condition and individual response:
- Simple habits or specific phobias: 1-4 sessions often sufficient
- Anxiety disorders: 4-8 sessions typically
- Chronic pain: Minimum 8 sessions for optimal outcomes [1]
- IBS (gut-directed hypnotherapy): 6-12 sessions standard protocol
- Complex presentations: 10-20 sessions may be needed
Choose longer protocols if: You're addressing chronic conditions, multiple interconnected issues, or conditions with strong research supporting extended treatment (like chronic pain requiring minimum 8 sessions).
How Can Professionals Build a Hypnotherapy Career or Practice?

Building a successful hypnotherapy practice requires combining clinical competence with business development skills, strategic positioning, and professional networking. The field offers multiple career pathways depending on your background, interests, and market positioning.
Career Pathways and Practice Models
Private practice: The most common model, offering flexibility and autonomy. Success requires strong marketing, business management, and client relationship skills. Initial client acquisition typically takes 6-18 months to build sustainable caseload.
Healthcare integration: Working within GP surgeries, pain clinics, gastroenterology departments, or hospitals. Requires building referral relationships with medical professionals and often additional credentials. Gastroenterologist referrals are increasing for IBS treatment as clinical guidelines gain awareness [1].
Corporate wellness: Providing stress management, performance enhancement, and resilience training to organizations. Requires adapting clinical approaches to workplace contexts and group delivery formats.
Specialized niche practice: Focusing on high-demand specializations like gut-directed hypnotherapy, chronic pain management, or pediatric applications. Specialists typically command higher fees and attract medical referrals more readily.
Teaching and training: Delivering hypnotherapy training programs once you've established substantial clinical experience (typically 5+ years and 500+ client hours).
Strategic Positioning in Growing Niches
The fastest-growing hypnotherapy niches in 2026 offer distinct advantages:
Gut-directed hypnotherapy provides the strongest medical referral potential due to gastroenterology guideline recommendations [1]. Practitioners report that healthcare provider referrals generate more committed clients with better outcomes.
Chronic pain management attracts clients seeking non-pharmacological alternatives to opioid medications. The minimum eight-session protocol requirement [1] creates more stable, longer-term client relationships than brief interventions.
Pediatric applications show some of the largest effect sizes [1] and create family-based referral networks. Parents whose children experience successful outcomes become strong advocates.
Performance anxiety applications span multiple markets: athletes, musicians, public speakers, executives. This diversity provides income stability across economic conditions.
Building Medical Referral Networks
Medical referrals represent the highest-quality client source, with better adherence and outcomes [1]. Building these relationships requires:
- Evidence-based positioning: Sharing relevant research and clinical guidelines with potential referring providers
- Clear communication: Providing regular progress updates to referring doctors (with client consent)
- Scope awareness: Knowing when to refer back to medical care and demonstrating clinical judgment
- Professional credentials: Maintaining registration with recognized bodies and relevant insurance
- Outcome tracking: Documenting client improvements using validated measures
Common mistake: Marketing hypnotherapy with exaggerated claims or "cure-all" messaging. Medical professionals respond to evidence-based, modest claims supported by research, not hyperbolic promises.
Essential Business Development Skills
Successful practice building requires competencies beyond clinical skills:
- Marketing fundamentals: Website development, search engine optimization, content marketing
- Relationship building: Networking with complementary practitioners and potential referral sources
- Financial management: Pricing strategy, expense tracking, tax compliance
- Client management: Scheduling systems, record-keeping, follow-up protocols
- Professional development: Staying current with research and advancing clinical skills
Understanding psychology and mental health therapy provides valuable context for positioning hypnotherapy within the broader therapeutic landscape.
What Are the Limitations and Contraindications of Hypnotherapy?
While hypnotherapy demonstrates excellent safety profiles with no significant adverse events reported across recent studies from 2018-2026 [3], certain limitations and contraindications require awareness for safe, ethical practice.
Clinical Contraindications
Absolute contraindications (hypnotherapy should not be used):
- Active psychosis: Schizophrenia, bipolar disorder in manic phase, or other conditions involving loss of reality testing
- Severe dissociative disorders: Conditions where trance states might exacerbate dissociation
- Epilepsy (relative): Requires medical clearance and caution, as deep relaxation may occasionally trigger seizures in susceptible individuals
Relative contraindications (proceed with caution and medical consultation):
- Severe depression with suicidal ideation: Requires concurrent psychiatric care
- Personality disorders: May require modified approaches and realistic outcome expectations
- Recent trauma: May require trauma-informed modifications to avoid retraumatization
- Cardiovascular conditions: Deep relaxation can affect blood pressure and heart rate
- Pregnancy: Generally safe but requires informed consent and appropriate positioning
Scope of Practice Limitations
Hypnotherapy is not appropriate as a standalone treatment for:
- Medical conditions requiring diagnosis and treatment by qualified physicians
- Serious mental health conditions requiring psychiatric intervention
- Dental procedures (unless the practitioner is a qualified dentist)
- Conditions outside the practitioner's training and competence
Common mistake: Practitioners working beyond their scope of competence. If you've trained in anxiety management but not trauma, referring trauma clients to appropriately qualified practitioners protects both client welfare and professional credibility.
Realistic Outcome Expectations
Hypnotherapy shows strong evidence for specific applications but is not universally effective:
- Individual variability: Approximately 10-15% of people show low hypnotic responsiveness, limiting technique effectiveness
- Motivation requirement: Clients must genuinely want to change; hypnotherapy cannot force unwanted changes
- Complementary role: Works best alongside, not replacing, conventional medical care for serious conditions
- Time requirements: Meaningful change typically requires multiple sessions, not single-session "cures"
Choose alternative or additional approaches if the client shows minimal hypnotic responsiveness after 2-3 sessions, lacks genuine motivation for change, or presents with conditions outside hypnotherapy's evidence base.
What Does Research Say About Hypnotherapy Effectiveness?
Recent systematic reviews and meta-analyses establish hypnotherapy as an evidence-based intervention with measurable clinical outcomes across multiple conditions. A 2019-2025 scoping review examining 1,250 records identified 30 studies meeting rigorous inclusion criteria, with hypnotherapy most frequently applied to IBS using gut-directed hypnotherapy as the predominant technique, resulting in better quality of life and reduced anxiety across psychosomatic conditions [2].
Neurological Evidence
Neurophysiological studies reveal that hypnotic analgesia has clear effects on brain and spinal-cord functioning, providing objective evidence beyond placebo [1]. Brain imaging demonstrates measurable changes in neural activity during hypnotic states, particularly in regions governing attention, sensory processing, and emotional regulation.
These findings counter skepticism about hypnotherapy being "just placebo." While placebo effects contribute to all therapeutic interventions, hypnotherapy produces specific neurological changes distinct from placebo responses alone.
Comparative Effectiveness
Hypnotherapy demonstrates outcomes comparable to or exceeding established treatments:
- Depression: Outcomes comparable to or exceeding cognitive behavioural therapy, with sustained benefits extending up to 3.5 years post-treatment [3]
- IBS: Equally effective as the low FODMAP diet for symptom management while being more effective at improving psychological measures [1]
- Chronic pain: Effect sizes ranging from medium to large (d = 0.5 to 2.72) across various pain conditions [3]
Safety Profile
No significant adverse events have been reported across studies from 2018-2026 [3], establishing hypnotherapy as one of the safest therapeutic interventions available. This safety profile makes hypnotherapy particularly valuable for populations where pharmaceutical interventions carry significant risks, such as children, pregnant women, and individuals with complex medication regimens.
Evidence Gaps and Ongoing Research
Despite strong evidence for specific applications, research gaps remain:
- Mechanism studies: More research needed on exactly how hypnotherapy produces clinical changes
- Predictive factors: Better identification of who responds best to which hypnotic approaches
- Optimal protocols: Refinement of session numbers, frequency, and technique combinations for specific conditions
- Long-term outcomes: More extended follow-up studies beyond current 3.5-year maximum [3]
Edge case: Absence of evidence is not evidence of absence. Limited research on certain applications (like hypnotherapy for specific rare conditions) doesn't mean ineffectiveness, just insufficient investigation. However, ethical practice requires basing claims on existing evidence, not speculation about unstudied applications.
Frequently Asked Questions About Hypnotherapy

Can anyone be hypnotized?
Most people can experience hypnotic trance to some degree, but responsiveness varies. Approximately 10-15% of people show high hypnotic responsiveness, 10-15% show low responsiveness, and the majority fall in the moderate range. Low responsiveness doesn't preclude benefit, but highly responsive individuals typically experience more dramatic results.
Will I lose control during hypnotherapy?
No. Hypnotherapy is a collaborative process where you remain aware and in control throughout. You cannot be made to do anything against your values or will. The hypnotic state resembles focused absorption, not unconsciousness or mind control.
How many sessions will I need?
This depends on your presenting issue. Simple phobias or habits may resolve in 1-4 sessions, anxiety typically requires 4-8 sessions, while chronic pain shows optimal outcomes with minimum 8 sessions [1]. Your hypnotherapist should provide realistic estimates during initial assessment.
Does hypnotherapy work for smoking cessation?
Evidence for smoking cessation is mixed. While some individuals report success, systematic reviews show less consistent outcomes compared to applications like IBS, anxiety, or chronic pain. Hypnotherapy for smoking works best when combined with genuine motivation to quit and often requires multiple sessions plus ongoing support.
Is hypnotherapy covered by insurance or the NHS?
NHS provision is limited but growing, particularly in pain clinics and some gastroenterology departments for IBS. Private insurance coverage varies by provider and policy. Check with your specific insurer. Most hypnotherapy in the UK is currently private pay.
What's the difference between a hypnotherapist and a hypnotist?
A hypnotherapist uses hypnosis for therapeutic purposes, requiring clinical training in assessment, treatment planning, and evidence-based interventions. A hypnotist may use hypnosis for entertainment (stage hypnosis) or limited applications without comprehensive therapeutic training. Always verify clinical qualifications and professional registration.
Can hypnotherapy recover repressed memories?
Memory recovery through hypnotherapy is controversial and potentially unreliable. Research shows hypnosis can increase confidence in memories without increasing accuracy, potentially creating false memories. Ethical practitioners avoid memory recovery work or use extreme caution with appropriate informed consent.
Is hypnotherapy safe for children?
Yes, when delivered by appropriately trained practitioners. Children often show excellent hypnotic responsiveness and demonstrate some of the largest effect sizes for applications like needle-related procedures and pre-surgical anxiety [1]. Pediatric hypnotherapy requires specialized training in child development and age-appropriate techniques.
How do I choose a qualified hypnotherapist?
Verify registration with recognized professional bodies (GHR, NCH, BSCH, or CNHC in the UK), check their training credentials and specializations, ask about experience with your specific issue, and ensure they carry professional indemnity insurance. Initial consultation should include thorough assessment and realistic outcome discussion.
Can I learn self-hypnosis?
Yes. Many hypnotherapists teach clients self-hypnosis techniques to practice between sessions and maintain benefits after treatment ends. Self-hypnosis enhances treatment outcomes and provides ongoing self-management tools. However, learning from a qualified practitioner ensures proper technique and safety.
What's the difference between hypnotherapy and meditation?
Both involve focused attention and relaxation, but hypnotherapy includes specific therapeutic suggestions and interventions targeting particular outcomes, while meditation typically focuses on present-moment awareness without directed change efforts. Hypnotherapy is goal-oriented treatment; meditation is typically a wellness practice.
Does hypnotherapy work for weight loss?
Evidence is moderate. Hypnotherapy may support weight loss when combined with dietary and exercise changes, particularly by addressing emotional eating, motivation, and habit change. It's not a standalone solution and works best as part of comprehensive weight management approaches. Realistic expectations are essential.
Conclusion
Hypnotherapy has evolved from a misunderstood practice into an evidence-based therapeutic modality now recommended in mainstream medical guidelines for conditions including irritable bowel syndrome, chronic pain, anxiety disorders, and perioperative care. With no significant adverse events reported across recent studies and effect sizes ranging from medium to large across multiple applications, hypnotherapy offers working professionals both a valuable clinical tool and a viable career pathway.
The strongest evidence supports applications in anxiety management (accounting for 52% of global demand), gut-directed hypnotherapy for IBS (now recognized in gastroenterology guidelines), chronic pain management (requiring minimum eight sessions for optimal outcomes), and pediatric procedures (showing some of the largest effect sizes). These evidence-based applications provide the most reliable foundation for professional practice and career development.
For those considering hypnotherapy training, success requires completing accredited programs (typically 120-450 hours), obtaining professional registration with recognized bodies, and potentially pursuing specialized training in high-demand niches. Career pathways include private practice, healthcare integration, corporate wellness, and specialized niche practices, each requiring distinct business development approaches alongside clinical competence.
The field continues expanding as medical professionals become more aware of clinical guidelines recommending hypnotherapy, particularly gastroenterologists referring IBS patients for gut-directed protocols. This growing medical acceptance, combined with increasing consumer preference for non-pharmacological interventions, positions hypnotherapy for continued professional growth.
Next steps for prospective clients: Research qualified practitioners registered with professional bodies, verify their experience with your specific condition, and schedule an initial consultation to assess fit and discuss realistic outcomes.
Next steps for professionals considering training: Explore accredited training programs aligned with your interests and background, consider which specializations match growing market demand, and develop both clinical competencies and business development skills. Understanding psychology and mental health therapy provides valuable context, while building essential professional skills supports practice development alongside clinical expertise.
The convergence of robust research evidence, mainstream medical acceptance, and growing public awareness creates unprecedented opportunities for qualified hypnotherapy practitioners who combine clinical excellence with professional credibility and evidence-based practice.
References
[1] 5 Hypnotherapy Niches Growing Fastest 2026 - https://hypnosistrainingacademy.com/5-hypnotherapy-niches-growing-fastest-2026/
[2] 14 926 - https://f1000research.com/articles/14-926
[3] Preprints202602.0874 - https://sciety.org/articles/activity/10.20944/preprints202602.0874.v1










